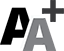A silver lining to the inconvenience of a mild COVID-19 infection is that for most people it is followed by a honeymoon period – an idyllic time when the immune system is firing on all cylinders and preventing reinfection.

Infection with omicron doesn’t protect as well as vaccination does. Charles Krupa/Associated Press, File
But all good things must come to an end. At some point, the surge of protective antibodies wanes.
With each new variant, that period of protection keeps getting shorter. In the past few weeks, studies out of South Africa, the United States and China have revealed that omicron subvariants BA.2.12.1, BA.4 and BA.5 are alarmingly good at escaping immunity from a previous omicron infection.
In practical terms, this means that for the large swath of the U.S. population that was first infected with COVID over the winter, the post-infection honeymoon may be over. Those people might wonder how safe it is to travel, attend large gatherings and have dinner with vulnerable friends and relatives.
Unfortunately, there are no easy answers. “People want it to be, ‘Am I safe or not?’ ” says Abraar Karan, an epidemiologist at Stanford University. But risk is a continuum.
That’s because at this stage in the pandemic, the variables are so complex and the data so limited (particularly in the U.S., where at-home tests have made it harder to keep tabs on spread of the virus), it’s impossible to pin down how long any individual’s immunity might last.
Scientists do have one concrete piece of evidence: Unvaccinated people who have been infected with omicron get very little protection against sublineages of that virus. A South African study revealed a wide gap between vaccinated and unvaccinated people in the amount of antibodies generated after an omicron infection.
“Bottom line is that omicron is really not a great vaccine,” says Alex Sigal, the virologist who led the study at the Africa Health Research Institute.
Sigal’s research showed that vaccinated people who have contracted omicron and thus have what scientists refer to as hybrid immunity do see at least a short-term rise in antibodies that can protect against earlier variants, such as delta, and, to a lesser extent, against omicron relatives such as BA.4 and BA.5.
So how often are reinfections happening in people with hybrid immunity? While health experts initially thought they were rare, emerging state-level data suggest they could be becoming more common.
Of the many virologists and epidemiologists I asked to assess the length of time that a vaccinated, then omicron-infected person can feel reasonably safe from a second round of COVID, most suggested anywhere from two to six months. But public health experts also point out that, in rare cases, people are getting reinfected within weeks. In this pandemic, there is no such thing as guaranteed protection.
There is at least a decent chance that subsequent infections in people with hybrid immunity will be less severe, as the immune system gets better at responding to the virus. But it’s worth remembering that public health experts still don’t know whether repeated infections might increase the risk of long COVID or other health consequences.
Given how haphazard infection tracking has become, it will be difficult to get a clear picture of those risks.
It’s yet another reminder of COVID’s staying power. Humanity may be ready to move on, but the coronavirus is holding its ground.
Send questions/comments to the editors.